Acute scaphoid fracturesThe scaphoid is the most commonly fractured wrist (carpal) bone constituting 60% of carpal fractures and 11% of all hand fractures. The fractures are particularly common in the 18 – 40 year age group and are a frequent cause of time off sport and debility. They are problematic fractures with a poor outcome if missed or inadequately treated.
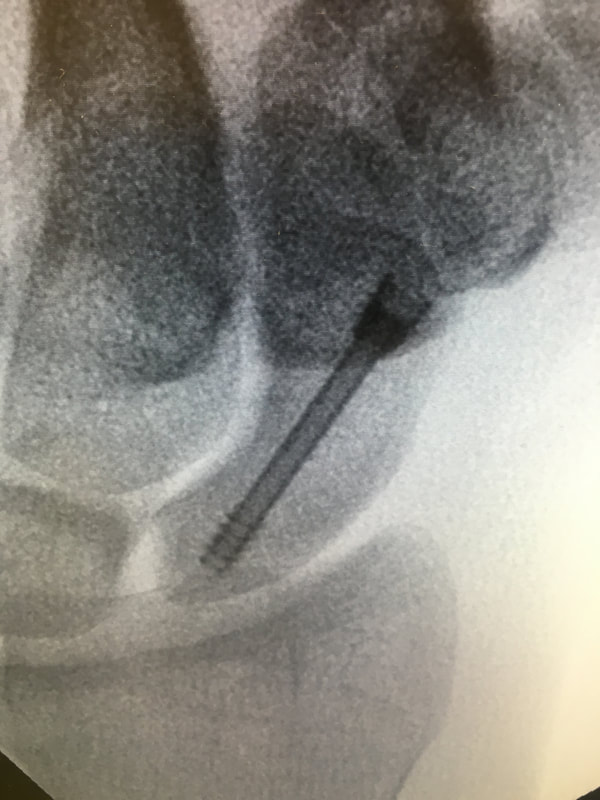
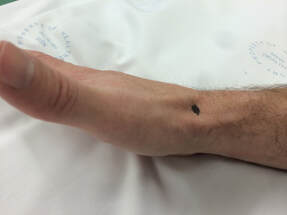
Most scaphoid fractures occur from a fall onto the outstretched hand but can also be from a punching injury. The injury is commonly misdiagnosed as a wrist sprain leading to the fracture not healing (non-union) and late presentation with persistent wrist pain and secondary arthritis due to abnormal kinematics (movement) in the carpus. To add to the complexity of treating these fractures, 25% - 50% of these fractures cannot be seen on the initial X-ray and the diagnosis is therefore based on clinical suspicion and a high level of vigilance by medical staff. After a fall, swelling and pain in the wrist should be considered a fracture (or severe ligament injury) until proven otherwise. Swelling and tenderness is usually maximal in the ‘anatomical snuffbox’(Figure 1), an area on the radial side of the wrist named from the (hopefully) historical habit of sniffing tobacco or ‘Snuff’ from the region! CT or MRI scans are frequently required to make the diagnosis and/or plan treatment. A CT scan shows the anatomy and pattern of the fracture much more clearly, but will occasionally (1-2%) still miss the fracture. MRI is more sensitive and has the advantage of showing ligament injuries but is less useful for planning treatment and I therefore usually start with a CT scan. The scaphoid is a ‘bean shaped’ bone, which is almost completely covered by articular cartilage and therefore has a poor blood supply, which can be further disrupted by a fracture. (Figure 2) The blood supply is retrograde, meaning the proximal part of the bone (proximal pole) has the poorest blood supply making fractures of this area the most problematic and least likely to heal. In my experience, proximal pole fractures are also the type of fracture that are least painful and are therefore more commonly self diagnosed as a ‘wrist sprain’. The literature clearly shows that all proximal pole fractures should be fixed internally (with a headless bone screw) as plaster treatment is prolonged and usually has a poor outcome. Conversely, distal pole fractures have a good outcome, resulting from their comparatively better blood supply. They generally only require cast immobilization (for 6 weeks) and the only indication for surgery is a significant intra-articular step in the scapho- trapezium joint which is uncommon. More common than both of the above are waist fractures, through the middle of the bone. These require surgery if there is any displacement of the fracture; this indicates a higher energy injury with a corresponding high risk of non-union with cast treatment alone. Undisplaced waist fractures can be treated in a cast for 8 to 12 weeks (Figure 3) with the majority healing (>95%). Usual return to contact sport is around 3 to 4 months post injury and if the fracture fails to heal bone graft (from the iliac crest) along with internal fixation is required. A quicker and more reliable recovery can be achieved by percutaneous screw fixation. Through a 5mm incision and under X-ray guidance a headless bone screw is inserted into the scaphoid and across the fracture. This has the advantage of allowing immediate wrist mobilization and quicker recovery with most people returning to contact sports 6 to 8 weeks after fracture. (Figure 4) Although this technique can be technically demanding for the surgeon, for an experienced wrist surgeon the complication rate is extremely low with a success rate close to 100%. Figure 1. Anatomic snuffbox Fig 2. Scaphoid vascular supply Fig 3. Well applied scaphoid cast Fig 4. Range of motion 6 weeks percutaneous screw fixation
|
|
|